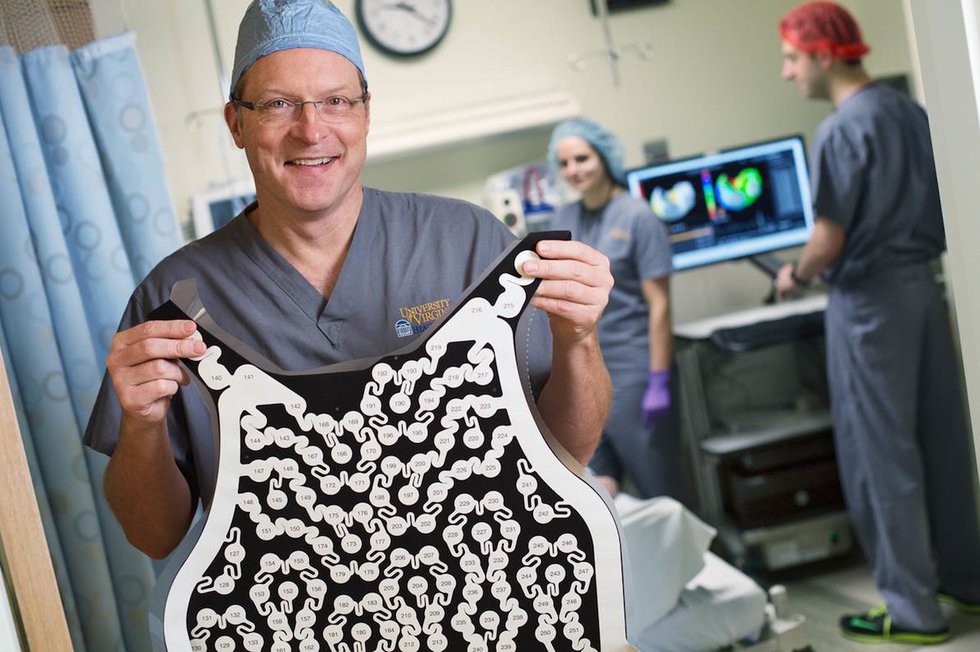
UVA electrophysiologists use new electrode technology to pinpoint source of AFib.

Dr. Mike Mangrum with CardioInsight Mapping Vest.
Photo courtesy of UVA
A cardiac mapping vest is helping physicians better track and treat atrial fibrillation (AFib), an arrhythmia in the upper chambers of the heart that affects about 3 million people in the U.S. each year.
The Atrial Fibrillation Center at UVA was the second facility in the U.S. to acquire Medtronic’s CardioInsight Mapping Vest, thanks to a $450,000 grant from the Seraph Foundation. “We did our first case [using the vest] on Feb. 1, 2017. We’ve had good results from it, and we are the leading center in the U.S. with this technology,” says Dr. Mike Mangrum, an electrophysiologist and director of the center, which draws about 3,000 patients from across the U.S. and world each year.
AFib patients often experience a “fluttering” feeling in the chest resulting from electrical miscues in the atrium that cause heart palpitations and irregular or rapid heartbeats. The condition makes them more prone to strokes. “What happens is, when you’re in AFib, the top chamber kind of quivers and blood can clot in the heart, embolize, and cause a stroke,” says Mangrum. “Blood thinners are usually tried first, and if patients don’t respond to medication, that’s when they come in for ablations.”
In an ablation, a doctor uses a special catheter to make small burns on the heart at the site of the misfiring. The resulting scar tissue prevents the atrium from sending further faulty electrical impulses to the ventricles. Before the ablation, the heart’s electrical signals are carefully mapped—something usually done by placing catheters on the patient’s heart.
As a less invasive option, UVA doctors can now use the Medtronic vests, which are disposable and made for one-time use. Numbers on the vest indicate the location of each electrode. Patients undergo a CT scan with the vest on “to create a 3D image of the atrium,” says Mangrum. “From the 252 electrodes, mathematically we can interpolate about 1,500 different points on the cardiac chamber.” This allows for a more exact identification of problem areas—including some that “were difficult, if not impossible, to locate before,” he says. Instead of a lab, the patient lies on a bed in a procedure room. “The family members can stay in the room where we do the mapping,” says Mangrum. “Patients love it.”
The vests may have future applications. Very early trials are being done using radiation to treat patients with persistent arrhythmias that do not respond to ablations. When using this new treatment, combined with the vests for mapping, “You could have an entire procedure that is non-invasive,” he says. “We’re very fortunate to be on the cutting edge of a technology that has that potential.” UVAHealth.com
This article originally appeared in our December 2018 issue.